 W
WNeurotrauma, brain damage or brain injury (BI) is the destruction or degeneration of brain cells. Brain injuries occur due to a wide range of internal and external factors. In general, brain damage refers to significant, undiscriminating trauma-induced damage, while neurotoxicity typically refers to selective, chemically induced neuron damage.
 W
WNerve injury is injury to nervous tissue. There is no single classification system that can describe all the many variations of nerve injury. In 1941, Seddon introduced a classification of nerve injuries based on three main types of nerve fiber injury and whether there is continuity of the nerve. Usually, however, (peripheral) nerve injury is classified in five stages, based on the extent of damage to both the nerve and the surrounding connective tissue, since supporting glial cells may be involved. Unlike in the central nervous system, neuroregeneration in the peripheral nervous system is possible. The processes that occur in peripheral regeneration can be divided into the following major events: Wallerian degeneration, axon regeneration/growth, and nerve reinnervation. The events that occur in peripheral regeneration occur with respect to the axis of the nerve injury. The proximal stump refers to the end of the injured neuron that is still attached to the neuron cell body; it is the part that regenerates. The distal stump refers to the end of the injured neuron that is still attached to the end of the axon; it is the part of the neuron that will degenerate but that remains in the area toward which the regenerating axon grows. The study of peripheral nerve injury began during the American Civil War and has greatly expanded to the point of using growth-promoting molecules.
 W
WClassification of peripheral nerve injury assists in prognosis and determination of treatment strategy. Classification of nerve injury was described by Seddon in 1943 and by Sunderland in 1951. The lowest degree of nerve injury in which the nerve remains intact but signaling ability is damaged is called neurapraxia. The second degree in which the axon is damaged but the surrounding connecting tissue remains intact is called axonotmesis. The last degree in which both the axon and connective tissue are damaged is called neurotmesis.
 W
WA brachial plexus injury (BPI), also known as brachial plexus lesion, is an injury to the brachial plexus, the network of nerves that conducts signals from the spinal cord to the shoulder, arm and hand. These nerves originate in the fifth, sixth, seventh and eighth cervical (C5–C8), and first thoracic (T1) spinal nerves, and innervate the muscles and skin of the chest, shoulder, arm and hand.
 W
WNeurotrauma, brain damage or brain injury (BI) is the destruction or degeneration of brain cells. Brain injuries occur due to a wide range of internal and external factors. In general, brain damage refers to significant, undiscriminating trauma-induced damage, while neurotoxicity typically refers to selective, chemically induced neuron damage.
 W
WBrain herniation is a potentially deadly side effect of very high pressure within the skull that occurs when a part of the brain is squeezed across structures within the skull. The brain can shift across such structures as the falx cerebri, the tentorium cerebelli, and even through the foramen magnum. Herniation can be caused by a number of factors that cause a mass effect and increase intracranial pressure (ICP): these include traumatic brain injury, intracranial hemorrhage, or brain tumor.
 W
WCauda equina syndrome (CES) is a condition that occurs when the bundle of nerves below the end of the spinal cord known as the cauda equina is damaged. Signs and symptoms include low back pain, pain that radiates down the leg, numbness around the anus, and loss of bowel or bladder control. Onset may be rapid or gradual.
 W
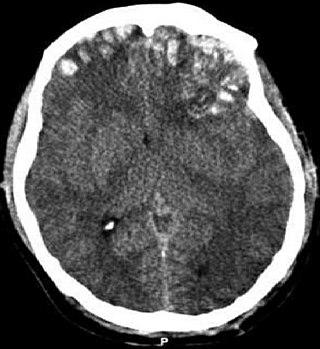
WCerebral contusion, Latin contusio cerebri, a form of traumatic brain injury, is a bruise of the brain tissue. Like bruises in other tissues, cerebral contusion can be associated with multiple microhemorrhages, small blood vessel leaks into brain tissue. Contusion occurs in 20–30% of severe head injuries. A cerebral laceration is a similar injury except that, according to their respective definitions, the pia-arachnoid membranes are torn over the site of injury in laceration and are not torn in contusion. The injury can cause a decline in mental function in the long term and in the emergency setting may result in brain herniation, a life-threatening condition in which parts of the brain are squeezed past parts of the skull. Thus treatment aims to prevent dangerous rises in intracranial pressure, the pressure within the skull.
 W
WIntracerebral hemorrhage (ICH), also known as cerebral bleed, is a type of intracranial bleed that occurs within the brain tissue or ventricles. Symptoms can include headache, one-sided weakness, vomiting, seizures, decreased level of consciousness, and neck stiffness. Often symptoms get worse over time. Fever is also common. In many cases bleeding is present in both the brain tissue and the ventricles.
 W
WChildhood acquired brain injury (ABI) is the term given to any injury to the brain that occurs during childhood but after birth and the immediate neonatal period. It excludes injuries sustained as a result of genetic or congenital disorder. It also excludes those resulting from birth traumas such as hypoxia or conditions such as foetal alcohol syndrome. It encompasses both traumatic and non-traumatic injuries.
 W
WChronic traumatic encephalopathy (CTE) is a neurodegenerative disease which causes severe and irreparable brain damage, as a result of repeated head injuries. Symptoms do not typically begin until years after the injuries and can include behavioral problems, mood problems, and problems with thinking. The disease often gets worse over time and can result in dementia. It is unclear if the risk of suicide is altered.
 W
WCognitive rehabilitation refers to a wide range of evidence-based interventions designed to improve cognitive functioning in brain-injured or otherwise cognitively impaired individuals to restore normal functioning, or to compensate for cognitive deficits. It entails an individualized program of specific skills training and practice plus metacognitive strategies. Metacognitive strategies include helping the patient increase self-awareness regarding problem-solving skills by learning how to monitor the effectiveness of these skills and self-correct when necessary.
 W
WConcussion, also known as mild traumatic brain injury (mTBI), is a head injury that temporarily affects brain functioning. Symptoms may include loss of consciousness (LOC); memory loss; headaches; difficulty with thinking, concentration or balance; nausea; blurred vision; sleep disturbances; and mood changes. Any of these symptoms may begin immediately, or appear days after the injury. Concussion should be suspected if a person indirectly or directly hits their head and experiences any of the symptoms of concussion. It is not unusual for symptoms to last 2 weeks in adults and 4 weeks in children. Fewer than 10% of sports-related concussions among children are associated with loss of consciousness.
 W
WIn head injury, a coup injury occurs under the site of impact with an object, and a contrecoup injury occurs on the side opposite the area that was hit. Coup and contrecoup injuries are associated with cerebral contusions, a type of traumatic brain injury in which the brain is bruised. Coup and contrecoup injuries can occur individually or together. When a moving object impacts the stationary head, coup injuries are typical, while contrecoup injuries are produced when the moving head strikes a stationary object.
 W
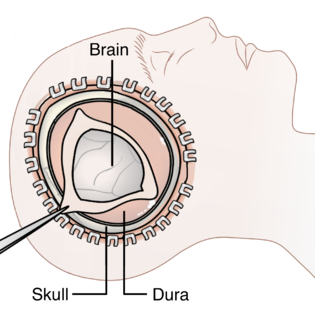
WDecompressive craniectomy is a neurosurgical procedure in which part of the skull is removed to allow a swelling brain room to expand without being squeezed. It is performed on victims of traumatic brain injury, stroke, Chiari Malformation, and other conditions associated with raised intracranial pressure. Use of the surgery is controversial.
 W
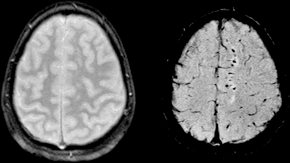
WDiffuse axonal injury (DAI) is a brain injury in which scattered lesions occur over a widespread area in white matter tracts as well as grey matter. DAI is one of the most common and devastating types of traumatic brain injury and is a major cause of unconsciousness and persistent vegetative state after severe head trauma. It occurs in about half of all cases of severe head trauma and may be the primary damage that occurs in concussion. The outcome is frequently coma, with over 90% of patients with severe DAI never regaining consciousness. Those who do wake up often remain significantly impaired.
 W
WThe Diving Bell and the Butterfly is a memoir by journalist Jean-Dominique Bauby. It describes his life before and after suffering a massive stroke that left him with locked-in syndrome.
 W
WEpidural hematoma is when bleeding occurs between the tough outer membrane covering the brain and the skull. Often there is loss of consciousness following a head injury, a brief regaining of consciousness, and then loss of consciousness again. Other symptoms may include headache, confusion, vomiting, and an inability to move parts of the body. Complications may include seizures.
 W
WIn excitotoxicity, nerve cells suffer damage or death when the levels of otherwise necessary and safe neurotransmitters such as glutamate, α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid (AMPA), or N-methyl-D-aspartic acid (NMDA) become pathologically high resulting in excessive stimulation of receptors. For example, when glutamate receptors such as the NMDA receptor or AMPA receptor encounter excessive levels of the excitatory neurotransmitter glutamate significant neuronal damage might ensue. Excess glutamate allows high levels of calcium ions (Ca2+) to enter the cell. Ca2+ influx into cells activates a number of enzymes, including phospholipases, endonucleases, and proteases such as calpain. These enzymes go on to damage cell structures such as components of the cytoskeleton, membrane, and DNA. In evolved, complex adaptive systems such as biologic life it must be understood that mechanisms are rarely, if ever, simplistically direct. For example, NMDA in subtoxic amounts induces neuronal survival to otherwise toxic levels of glutamate.
 W
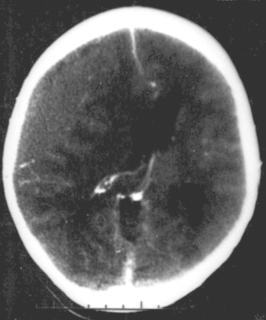
WFocal and diffuse brain injury are ways to classify brain injury: focal injury occurs in a specific location, while diffuse injury occurs over a more widespread area. It is common for both focal and diffuse damage to occur as a result of the same event; many traumatic brain injuries have aspects of both focal and diffuse injury. Focal injuries are commonly associated with an injury in which the head strikes or is struck by an object; diffuse injuries are more often found in acceleration/deceleration injuries, in which the head does not necessarily contact anything, but brain tissue is damaged because tissue types with varying densities accelerate at different rates. In addition to physical trauma, other types of brain injury, such as stroke, can also produce focal and diffuse injuries. There may be primary and secondary brain injury processes.
 W
WThe frontal lobe of the human brain is both relatively large in mass and less restricted in movement than the posterior portion of the brain. It is a component of the cerebral system, which supports goal directed behavior. This lobe is often cited as the part of the brain responsible for the ability to decide between good and bad choices, as well as recognize the consequences of different actions. Because of its location in the anterior part of the head, the frontal lobe is arguably more susceptible to injuries. Following a frontal lobe injury, an individual’s abilities to make good choices and recognize consequences are often impaired. Memory impairment is another common effect associated with frontal lobe injuries, but this effect is less documented and may or may not be the result of flawed testing. Damage to the frontal lobe can cause increased irritability, which may include a change in mood and an inability to regulate behavior. Particularly, an injury of the frontal lobe could lead to deficits in executive function, such as anticipation, goal selection, planning, initiation, sequencing, monitoring, and self-correction. A widely reported case of frontal lobe injury was that of Phineas Gage, a railroad worker whose left frontal lobe was damaged by a large iron rod in 1848.
 W
WGourmand syndrome is a very rare and benign eating disorder that usually occurs six to twelve months after an injury to the frontal lobe. Those with the disorder usually have suffered from a right hemisphere frontal or temporal brain lesion typically affecting the cortical areas, basal ganglia or limbic structures. These people develop a new, post-injury passion for gourmet food.
 W
WA head injury is any injury that results in trauma to the skull or brain. The terms traumatic brain injury and head injury are often used interchangeably in the medical literature. Because head injuries cover such a broad scope of injuries, there are many causes—including accidents, falls, physical assault, or traffic accidents—that can cause head injuries.
 W
WIntracranial hemorrhage (ICH), also known as intracranial bleed, is bleeding within the skull. Subtypes are intracerebral bleeds, subarachnoid bleeds, epidural bleeds, and subdural bleeds.
 W
WIntracranial pressure (ICP) is the pressure exerted by fluids such as cerebrospinal fluid (CSF) inside the skull and on the brain tissue. ICP is measured in millimeters of mercury (mmHg) and, at rest, is normally 7–15 mmHg for a supine adult. The body has various mechanisms by which it keeps the ICP stable, with CSF pressures varying by about 1 mmHg in normal adults through shifts in production and absorption of CSF.
 W
WPressure reactivity index or PRx is tool for monitoring cerebral autoregulation in the intensive care setting for patients with severe traumatic brain injury or subarachnoid haemorrhage, in order to guide therapy to protect the brain from dangerously high or low cerebral blood flow.
 W
WIntraparenchymal hemorrhage (IPH) is one form of intracerebral bleeding in which there is bleeding within brain parenchyma. The other form is intraventricular hemorrhage (IVH).
 W
WIntraventricular hemorrhage (IVH), also known as intraventricular bleeding, is a bleeding into the brain's ventricular system, where the cerebrospinal fluid is produced and circulates through towards the subarachnoid space. It can result from physical trauma or from hemorrhagic stroke.
 W
WLeague of Denial is a 2013 book, initially broadcast as a documentary film, about traumatic brain injury in the National Football League (NFL), particularly concussions and chronic traumatic encephalopathy (CTE). The documentary, entitled League of Denial: The NFL's Concussion Crisis, was produced by Frontline and broadcast on PBS. The book was written by ESPN reporters Mark Fainaru-Wada and Steve Fainaru. The book and film devote significant attention to the story of Mike Webster and his football-related brain injuries, and the pathologist who examined Webster's brain, Bennet Omalu. The film also looks closely at the efforts of researchers led by Ann McKee at Boston University's Center for the Study of Traumatic Encephalopathy, where the brains of a number of former NFL athletes have been examined.
 W
WLocked-in syndrome (LIS), also known as pseudocoma, is a condition in which a patient is aware but cannot move or communicate verbally due to complete paralysis of nearly all voluntary muscles in the body except for vertical eye movements and blinking. The individual is conscious and sufficiently intact cognitively to be able to communicate with eye movements. Electroencephalography results are normal in locked-in syndrome. Total locked-in syndrome, or completely locked-in state (CLIS), is a version of locked-in syndrome wherein the eyes are paralyzed as well. Fred Plum and Jerome Posner coined the term for this disorder in 1966.
 W
WMidline shift is a shift of the brain past its center line. The sign may be evident on neuroimaging such as CT scanning. The sign is considered ominous because it is commonly associated with a distortion of the brain stem that can cause serious dysfunction evidenced by abnormal posturing and failure of the pupils to constrict in response to light. Midline shift is often associated with high intracranial pressure (ICP), which can be deadly. In fact, midline shift is a measure of ICP; presence of the former is an indication of the latter. Presence of midline shift is an indication for neurosurgeons to take measures to monitor and control ICP. Immediate surgery may be indicated when there is a midline shift of over 5 mm. The sign can be caused by conditions including traumatic brain injury,stroke, hematoma, or birth deformity that leads to a raised intracranial pressure.
 W
WA minimally conscious state (MCS) is a disorder of consciousness distinct from persistent vegetative state and locked-in syndrome. Unlike persistent vegetative state, patients with MCS have partial preservation of conscious awareness. MCS is a relatively new category of disorders of consciousness. The natural history and longer term outcome of MCS have not yet been thoroughly studied. The prevalence of MCS was estimated to be 112,000 to 280,000 adult and pediatric cases.
 W
WNeurocritical care is a medical field that treats life-threatening diseases of the nervous system and identifies, prevents/treats secondary brain injury.
 W
WNMDA receptor antagonists are a class of drugs that work to antagonize, or inhibit the action of, the N-Methyl-D-aspartate receptor (NMDAR). They are commonly used as anesthetics for animals and humans; the state of anesthesia they induce is referred to as dissociative anesthesia.
 W
WOlney's lesions, also known as NMDA receptor antagonist neurotoxicity (NAN), are a form of potential brain damage due to drugs that have been studied experimentally and have produced neuronal damage, yet are administered by doctors to humans in the settings of pharmacotherapy and of anesthesia. They are named after John Olney, who conducted a study in 1989 to investigate neurotoxicity caused by PCP and related drugs. They are important for two reasons. Firstly, NMDA receptor antagonist are physician-prescribed drugs for therapeutic treatment of human diseases such as memantine for Alzheimer's disease and amantadine for Parkinson's disease, and also occur as street drugs that are taken recreationally. Secondly in the field of anesthesiology, the dissociative anesthesia of many general anesthetics is due to NMDA receptor antagonist properties. Because the neuronal vacuolation of Olney's lesions evolves into neuronal necrosis or death of neurons, it is important to determine whether Olney's lesions occur in humans, not only in experimental animals. The essential question is whether an NMDA receptor antagonist drug is to be considered a human neurotoxin or not. The patient safety implications for pharmacotherapy and for anesthesia would each be profound, if the answer is affirmative.
 W
WOpisthotonus or opisthotonos is a state of severe hyperextension and spasticity in which an individual's head, neck and spinal column enter into a complete "bridging" or "arching" position.
 W
WChildhood acquired brain injury (ABI) is the term given to any injury to the brain that occurs during childhood but after birth and the immediate neonatal period. It excludes injuries sustained as a result of genetic or congenital disorder. It also excludes those resulting from birth traumas such as hypoxia or conditions such as foetal alcohol syndrome. It encompasses both traumatic and non-traumatic injuries.
 W
WA penetrating head injury, or open head injury, is a head injury in which the dura mater, the outer layer of the meninges, is breached. Penetrating injury can be caused by high-velocity projectiles or objects of lower velocity such as knives, or bone fragments from a skull fracture that are driven into the brain. Head injuries caused by penetrating trauma are serious medical emergencies and may cause permanent disability or death.
 W
WSpinal locomotion results from intricate dynamic interactions between a central program in lower thoracolumbar spine and proprioceptive feedback from body in the absence of central control by brain as in complete spinal cord injury (SCI). Following SCI, the spinal circuitry below the lesion site does not become silent rather it continues to maintain active and functional neuronal properties although in a modified manner.
 W
WAlthough spinal cord injury (SCI) often causes sexual dysfunction, many people with SCI are able to have satisfying sex lives. Physical limitations acquired from SCI affect sexual function and sexuality in broader areas, which in turn has important effects on quality of life. Damage to the spinal cord impairs its ability to transmit messages between the brain and parts of the body below the level of the lesion. This results in lost or reduced sensation and muscle motion, and affects orgasm, erection, ejaculation, and vaginal lubrication. More indirect causes of sexual dysfunction include pain, weakness, and side effects of medications. Psycho-social causes include depression and altered self-image. Many people with SCI have satisfying sex lives, and many experience sexual arousal and orgasm. People with SCI employ a variety of adaptations to help carry on their sex lives healthily, by focusing on different areas of the body and types of sexual acts. Neural plasticity may account for increases in sensitivity in parts of the body that have not lost sensation, so people often find newly sensitive erotic areas of the skin in erogenous zones or near borders between areas of preserved and lost sensation.
 W
WAbusive head trauma (AHT), commonly known as shaken baby syndrome (SBS), is an injury to a child's head caused by someone else. Symptoms may range from subtle to obvious. Symptoms may include vomiting or a baby that will not settle. Often there are no visible signs of trauma. Complications include seizures, visual impairment, cerebral palsy, and cognitive impairment.
 W
WA skull fracture is a break in one or more of the eight bones that form the cranial portion of the skull, usually occurring as a result of blunt force trauma. If the force of the impact is excessive, the bone may fracture at or near the site of the impact and cause damage to the underlying structures within the skull such as the membranes, blood vessels, and brain.
 W
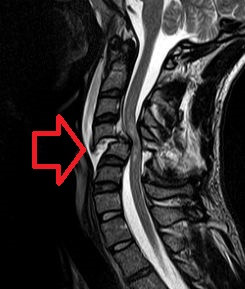
WA spinal cord injury (SCI) is damage to the spinal cord that causes temporary or permanent changes in its function. Symptoms may include loss of muscle function, sensation, or autonomic function in the parts of the body served by the spinal cord below the level of the injury. Injury can occur at any level of the spinal cord and can be complete, with a total loss of sensation and muscle function at lower sacral segments, or incomplete, meaning some nervous signals are able to travel past the injured area of the cord up to the Sacral S4-5 spinal cord segments. Depending on the location and severity of damage, the symptoms vary, from numbness to paralysis, including bowel or bladder incontinence. Long term outcomes also range widely, from full recovery to permanent tetraplegia or paraplegia. Complications can include muscle atrophy, loss of voluntary motor control, spasticity, pressure sores, infections, and breathing problems.
 W
WStill Me is a 1999 autobiography written by actor Christopher Reeve. The book tells of Reeve's experiences of making the Superman films and about his horseback riding accident which resulted in his quadriplegia and its effects on his life. The book spent eleven weeks on the New York Times Best Seller list in 1999. Reeve won a Grammy Award for Best Spoken Word Album.
 W
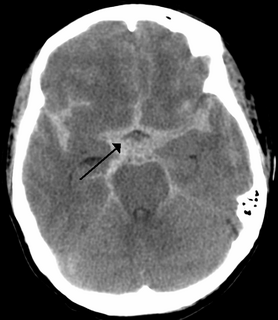
WSubarachnoid hemorrhage (SAH) is bleeding into the subarachnoid space—the area between the arachnoid membrane and the pia mater surrounding the brain. Symptoms may include a severe headache of rapid onset, vomiting, decreased level of consciousness, fever, and sometimes seizures. Neck stiffness or neck pain are also relatively common. In about a quarter of people a small bleed with resolving symptoms occurs within a month of a larger bleed.
 W
WA subdural hematoma (SDH) is a type of bleeding in which a collection of blood—usually associated with a traumatic brain injury—gathers between the inner layer of the dura mater and the arachnoid mater of the meninges surrounding the brain. It usually results from tears in bridging veins that cross the subdural space.
 W
WA traumatic brain injury (TBI), also known as an intracranial injury, is an injury to the brain caused by an external force. TBI can be classified based on severity, mechanism, or other features. Head injury is a broader category that may involve damage to other structures such as the scalp and skull. TBI can result in physical, cognitive, social, emotional and behavioral symptoms, and outcomes can range from complete recovery to permanent disability or death.
 W
WWallerian degeneration is an active process of degeneration that results when a nerve fiber is cut or crushed and the part of the axon distal to the injury degenerates. A related process of dying back or retrograde degeneration known as 'Wallerian-like degeneration' occurs in many neurodegenerative diseases, especially those where axonal transport is impaired such as ALS and Alzheimer's disease. Primary culture studies suggest that a failure to deliver sufficient quantities of the essential axonal protein NMNAT2 is a key initiating event.